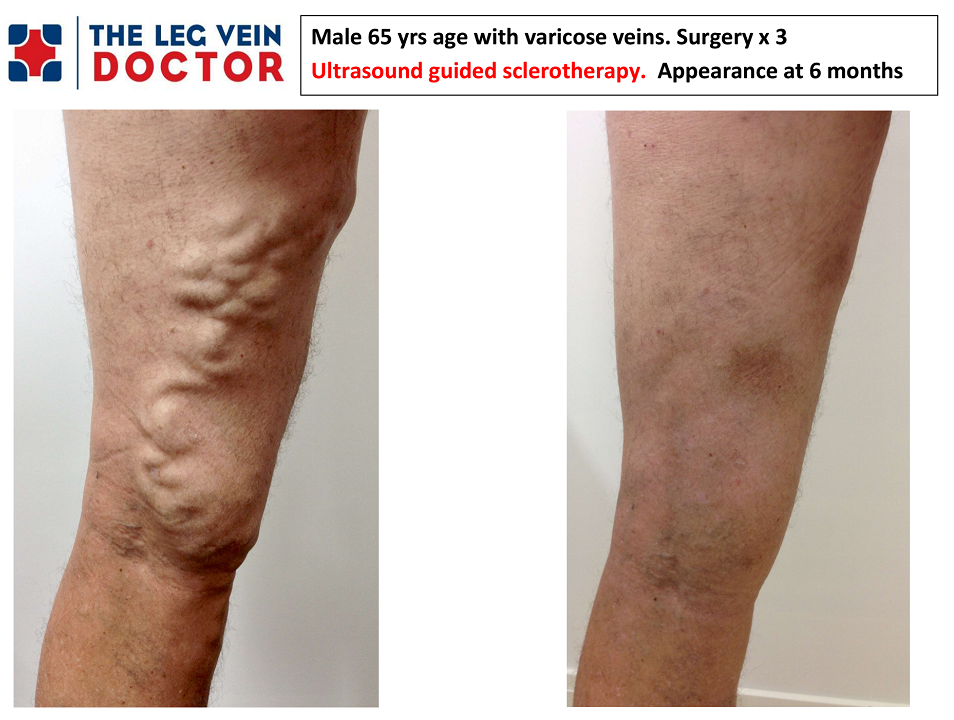
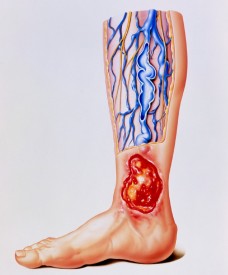
All you need to know about UGFS.
Read MoreDr Nicholas Kemp is a Specialist GP has post graduate Procedural Phlebology, Sclerotherapy and Ultrasound qualifications.
The Leg Vein Doctor offers treatments for varicose and spider veins in Brisbane and Toowoomba.
Read MoreAre you not coming for treatment of your spider veins because you are afraid of needles or pain? The Leg Vein Doctor in Brisbane and Toowoomba can help reassure you that treatment may not be as scary as you think.
Read MoreI just have surface veins do I need a scan?
Read More