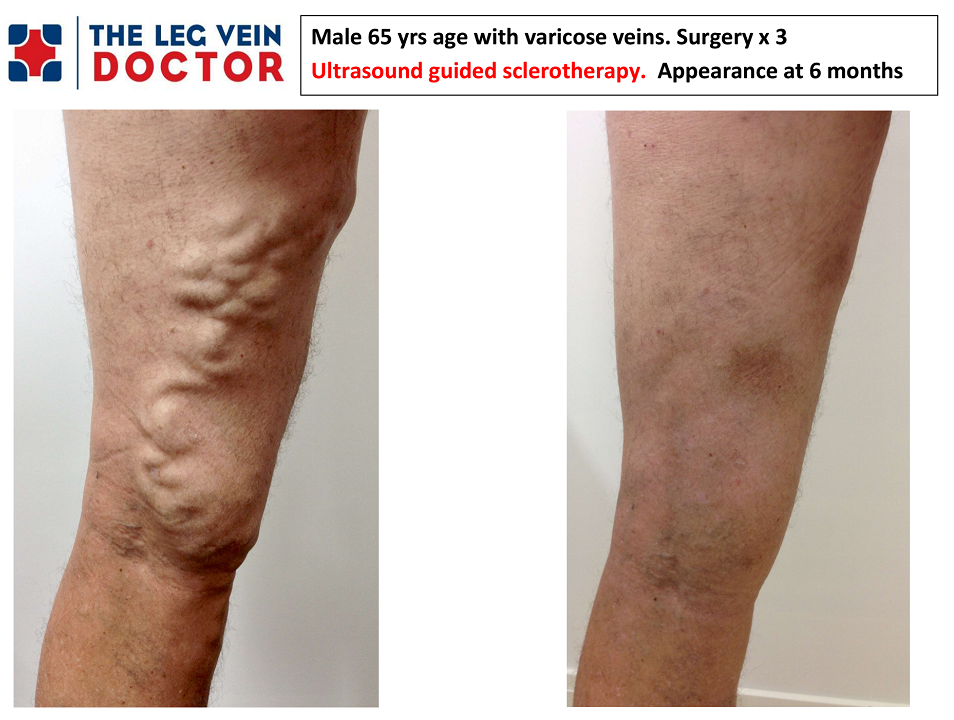
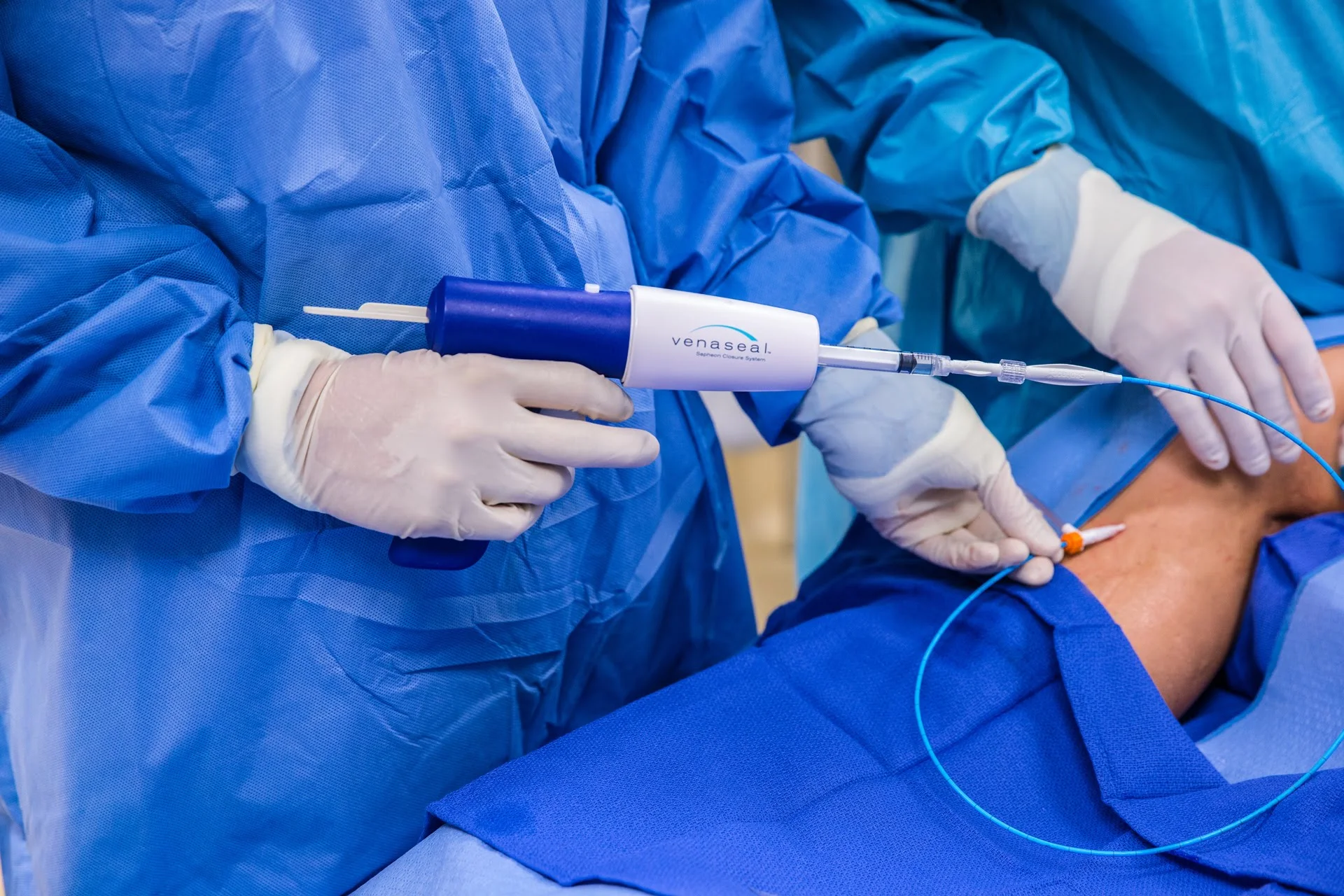
In this post Dr Nick Kemp discusses the reasons why May is a popular time to commence leg vein treatment.
Read MoreQueensland will be welcoming some of the worlds top Phlebologists later in the month with the 17th Annual Scientific Meeting (ASM) of the Australasian College of Phlebology (ACP) Conference on the Sunshine Coast.
Read More